Delayed cord clamping for 3 minutes or longer has long term benefits to the neonate, does NO harm and does not affect the mother in a negative way.
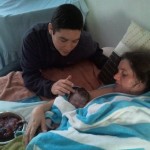
Conversely, immediate clamping of the umbilical cord leads to a higher incidence of anaemia or iron deficiency on infants at 4 months of age. Seeing that iron deficiency and lowered blood oxygen levels are associated with delays in early infant development, clamping and cutting the cord immediately after birth seems counterproductive and counter-intuitive. Physiological cord vessel closure occurs after the newborn baby’s lungs are inflated by the extra volume of blood transfused via the umbilical cord from the placenta. This capillary inflation stimulates the gasping reflex and the baby breathes. It is therefore expedient to allow the baby to remain level with the mother’s body for a few minutes after the birth.
But there are other concerns here: When 34% of women who die in childbirth in 3rd world countries and 13% of women (who die in childbirth) in developed countries are dying from post-partum haemorrhage, active management of the third stage of labour saves women’s lives. Active management of the third stage of labour is characterized by immediate cord clamping and administration of an intra-muscular injection of oxytocin. Most medical workers in and out of hospitals have, up till now, been encouraged to follow this protocol globally.
Immediate cord clamping is however detrimental to the newborn and developing infant. Clearly protocols need to be modified.
I recommend the following:
- A comprehensive medical, surgical history and nutritional status must be obtained from ALL pregnant women so as to establish what the risk may be of post-partum haemorrhage (PPH), such as history of haemophilia in the family, nose bleeds, haemorrhage with previous births, approximate expected size of the baby(large babies are associated with PPH), or pregnancy illness such as diabetes and Gestational Proteinuric Hypertension for example.
- Supplementing the mother’s diet with vitamins and minerals and sometimes herbal substances and ensure long term nutritional health by counselling about diet and lifestyle
- Establish what the risk might be of a long labour, exhaustion, large baby, twins etc and be prepared with an intravenous line in situ, Syntocinon or other uterotonics at the ready.
- If a mother is haemorrhaging, attend to this immediately, and establish the source. Sometimes bleeding is due to trauma of the pelvic floor and tearing, when the uterus is actually well contracted. Manual pressure is required in this instance and call for assistance. ‘Delaying cord clamping’ does not mean doing this at the expense of the mother.
- Physiological 3rd stage works best when mother and baby are NOT DISTURBED after the birth. Skin to skin and eye contact between mother and baby is ideal and elicits the release of maternal oxytocin which contracts the uterus and aids the expulsion of the placenta. In an article called “Don’t wake the Mother”, world famous obstetrician Dr Michel Odent documents reasons why mother and baby must be UNDISTURBED for the first hour after birth.
- It works even better if the mother initiates the first contact with her baby. In other words, allow the mother to touch and pick her baby up after birth rather than ‘hand’ the baby to her before she is ready to receive him.
- When a newborn requires resuscitation, attend to this BEFORE worrying about the cord or the placenta. The extra blood flow through the cord to the baby may mean the difference between life and death if a baby is compromised at birth. A hypovolaemic baby is much more difficult to resuscitate and stabilize than a baby with an adequate blood volume.
- Babies born by caesarian section can be laid next to the mother on the operating theatre table and covered with a warm blanket for 1-3 minutes before clamping and cutting the cord is implemented.

In practice I rarely cut the cord before the placenta is expelled. While some parents choose to cut the cord within the first hour of birth, some parents keep the placenta attached until it detaches spontaneously. This is called a lotus birth and it is best to keep the placenta in a salted container to delay decay. The cord dries, shrivels and falls off at the navel of the baby within a few days. The parents preferences around the rituals they may choose should be honoured. The important message here is DON’T CUT THE CORD for at the very least 3-5 minutes after the baby is born.
Erasmus Darwin, a doctor in the 19th century observed:
“Another thing very injurious to the child, is the tying and cutting of the navel string too soon; which should always be left till the child has not only repeatedly breathed but till all pulsation in the cord ceases. As otherwise the child is much weaker than it ought to be, a portion of the blood being left in the placenta, which ought to have been in the child” (Darwin E. (1801) Zoonomia, 3rd edition. London: vol III page 302).





Does anyone have statistics on how many lotus birth happen in various parts of the world?
Hi Sharon, Thanks for the question about Lotus births. Lotus birth is sort of an underground activity right now and it really depends on the midwife or midwives who attend births. A full Lotus birth is where the placenta and cord stay attached until the cord dries up and falls off spontaneously. This can take up to 5 days and mothers will often make a patchwork or embroidered bag in which to house the placenta with salt (in a plastic inner). But many women choose to keep the placenta attached in a bowl for anything from one hour to six hours or more and then cut the cord. This is also a form of lotus birth. The cord with turn completely white and dry. Most of the births I attended n the last 15 years were lotus births of one length or another. Thats about 1500 births. At Ibu Robin Lim’s birth centre in Bali Lotus birth is standard practice where possible. So I guess you need to ask individual midwives and then tally the numbers. Hope this helps.
C/section babies can have a Lotus Birth. There is no need to cut their cord. There are accounts of these births in the 2nd edition of lotus Birth. http://www.lotusbirth.net
Yes, Shivana, you are right. There is no reason why a C/section baby cannot have a lotus birth as well.
WHO recommends not less than one minute of placental transfusion in their new guidelines on PPH, published in 2012. http://www.who.int/ reproductivehealth/publications/maternal_perinatal_health/9789241548502/en/
What petition?
To be blessed and supported by the universe – is to be with Marianne as your midwife. And i mean that in the most grounded and practical terms.
We had – what is called an unassisted birth ; but that would have in no way been possible without the unrelenting support and guidance from Marianne. Leading up to and after our beautiful birthing experience – which was indeed a healing and astounding experience for us – Marianne was truly patient with such new parents-to-be 🙂 big appreciation !!!
Thank You Penelope. I will visit soon as have a few calmer days coming up!
Great article! I am currently a nursing student in the US and my instructors are less than enthusiastic about any birth that differs from a typical hospital delivery. It’s really discouraging to me as I want to be a nurse-midwife and help women bring their babies into the world in any way they choose. This is a great site for encouraging and educating mother! I look forward to reading many more great articles on this page!
Thanku Marianne ! Till the day I die I will promote natural third stage and natural childbirth!! As a powerful possibility for all womben
Love your articles and passion xxx
super article
Marianne